Benzodiazepine addiction often develops gradually, sometimes through a valid prescription, but over time, it takes a real toll. At Ojai Recovery, we offer trauma-informed treatment and medically supervised detox in a peaceful, supportive setting, helping you heal with dignity and rediscover a life beyond benzos.

2 reviews
3 months ago
This place has changed my life! I never envisioned having an awakening until I came to this place. It is the best place in Ventura County. They have the most amazing staff who go out of their way to be there for you I personally Experienced so much love from them..extra bonus best food ever!

1 review
2 months ago
As a parent, I am so grateful to Ojai Recovery. My son they did help when I was almost desperate. He’s just hit one year sober and is doing great.

62 reviews
A month ago
Beautiful property! Staff is absolutely amazing and will help anyway they can!! A++

1 review
2 months ago

1 review
A day ago
Benzodiazepine addiction, also known as Benzodiazepine Use Disorder, is a chronic condition where the brain becomes dependent on medications like Xanax, Valium, Klonopin, or Ativan to feel calm or function normally. What often begins as a prescription for anxiety, panic, or sleep can quietly shift into a physical and emotional dependence that feels impossible to stop.
It’s not a character flaw or a sign of weakness, it’s a medical condition rooted in brain chemistry and often intertwined with unresolved anxiety, trauma, or chronic stress. It deserves real treatment and real compassion.
You don’t have to figure this out by yourself. If any of these signs sound familiar, compassionate help is available. Reach out today to talk with a specialist and explore safe, supportive options for change.
Benzodiazepine withdrawal is one of the few forms of drug withdrawal that can be life-threatening without proper medical supervision. Understanding the risks is not meant to frighten you, it’s meant to emphasize that getting help sooner rather than later is one of the most important decisions you can make for yourself and the people who love you.
Risks include:
Dual diagnosis treatment is care that addresses both benzodiazepine addiction and an underlying mental health condition — like anxiety, depression, PTSD, or panic disorder — at the same time. For most people who develop benzo dependence, the two are deeply connected, and treating one without the other rarely leads to lasting recovery.
Dual diagnosis treatment is required when:
After detox and stabilization, clients transition into our full-time, campus-based addiction treatment residential program. This phase includes:
At Ojai Recovery, we know that healing from benzodiazepine addiction is about more than simply stopping a medication, it’s about understanding what the benzos were doing for you, and building healthier, lasting ways to feel safe and calm. Our approach blends evidence-based treatment with the natural serenity of Ojai, creating an environment where clients feel supported, seen, and empowered to recover.
A Place To Breathe, Heal, And Grow.
Our addiction recovery programs are designed to help you slow down, focus inward, and find balance. In the heart of Ojai’s natural beauty, you’ll experience an environment that nurtures both mind and body, with gentle mountain breezes, open skies, and quiet moments that remind you how steady and peaceful life can feel.
Your days here at our Addiction Treatment Center in Oak View, CA may begin with a walk along the shore of Casitas Lake, where the sunlight dances on the water and the air feels fresh with possibility. You might spend your afternoons in therapy, hiking shaded trails through the hills, journaling on a sunlit porch, or simply listening to the sounds of nature, a bird’s call, a rustling leaf, the soft hum of the wind.
Your Complete Wellness Matters.
We look at your whole health picture, mind, body, and spirit. At our treatment center in Ventura County, CA, we offer therapy, yoga, meditation, nutrition guidance, and life skills training. These tools help you build a strong foundation for lasting recovery.
Ojai Recovery’s Agoura Hills Program provides compassionate, comprehensive care for individuals and families seeking freedom from addiction. Designed to meet the unique needs of the local community, our program offers a full continuum of services, including medical detox, residential treatment, and outpatient support, so clients can access the right level of care at every stage of recovery.
We provide physician-led detox in a calming, secure environment to safely manage withdrawal symptoms and stabilize health.
Ojai Recovery is a private-pay facility that accepts most PPO insurance plans. We provide transparent cost structures and personalized guidance.
Clients participate in guided outdoor experiences that promote calm, reflection, and sensory regulation, utilizing Agoura Hills’ trails, open space, and natural beauty.
We build post-treatment support with:
Clients engage in a structured program that includes:
Our addiction recovery programs are designed to help you slow down, focus inward, and find balance. In the heart of Ojai’s natural beauty, you’ll experience an environment that nurtures both mind and body, with gentle mountain breezes, open skies, and quiet moments that remind you how good life can feel.
Your days here at our Addiction Treatment Center in Oak View, CA may begin with a walk along the shore of Casitas Lake, where the sunlight dances on the water and the air feels fresh with possibility. You might spend your afternoons hiking shaded trails that wind through the hills, journaling on a sunlit porch, or simply listening to the sounds of nature, a bird’s call, a rustling leaf, the soft hum of the wind.
We look at your whole health picture – mind, body, and spirit. At our Alcohol Detox in Ventura County, CA, we offer therapy, yoga, meditation, nutrition guidance, and life skills training. These tools help you build a strong foundation for lasting recovery.

Chronic drinking, binge drinking, or self-medicating with alcohol often masks deeper emotional pain. We offer medical detox and trauma-informed therapy to help clients safely stop drinking, and rediscover life without it.
From heroin to fentanyl to prescription painkillers, opioid addiction requires careful detox, medication-assisted care when appropriate, and strong emotional support to address the trauma that often drives use.

For those who feel emotionally dependent on cannabis, our program offers clarity, structure, and the chance to reconnect with purpose and energy beyond the haze.

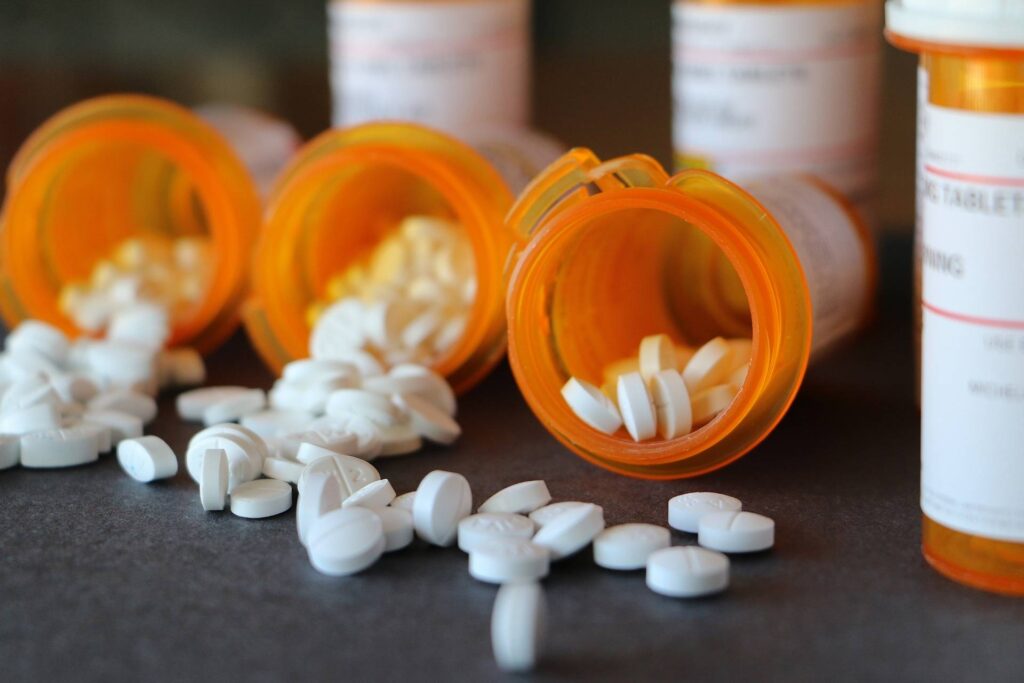
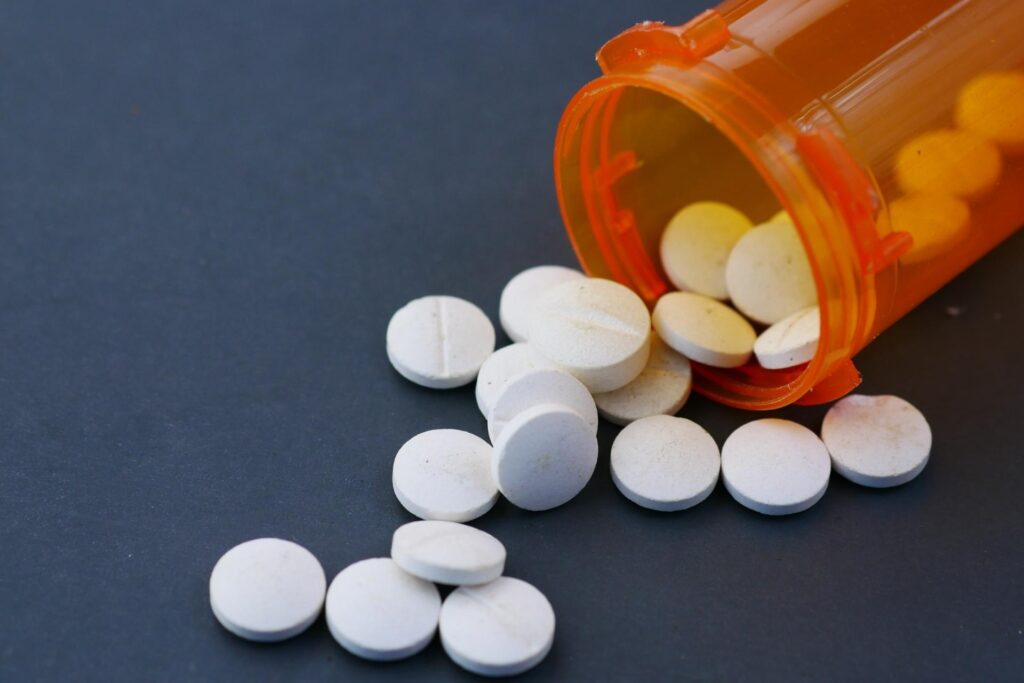
Whether painkillers, benzos, or ADHD medications, prescription drug misuse can quickly spiral into dependence. We treat this with clinical precision and deep compassion, focusing on both physical detox and emotional healing.
Cocaine, methamphetamine, and amphetamines can take a major toll on mental and emotional health. Our program helps clients rebuild from the psychological and neurological impact of long-term stimulant use.

For those facing both substance use and mental health challenges (like depression, anxiety, trauma, or bipolar disorder), we offer fully integrated care with licensed professionals who understand both sides of the story.

Chronic drinking, binge drinking, or self-medicating with alcohol often masks deeper emotional pain. We offer medical detox and trauma-informed therapy to help clients safely stop drinking, and rediscover life without it.

From heroin to fentanyl to prescription painkillers, opioid addiction requires careful detox, medication-assisted care when appropriate, and strong emotional support to address the trauma that often drives use.

For those who feel emotionally dependent on cannabis, our program offers clarity, structure, and the chance to reconnect with purpose and energy beyond the haze.

Whether painkillers, benzos, or ADHD medications, prescription drug misuse can quickly spiral into dependence. We treat this with clinical precision and deep compassion, focusing on both physical detox and emotional healing.

Cocaine, methamphetamine, and amphetamines can take a major toll on mental and emotional health. Our program helps clients rebuild from the psychological and neurological impact of long-term stimulant use.

For those facing both substance use and mental health challenges (like depression, anxiety, trauma, or bipolar disorder), we offer fully integrated care with licensed professionals who understand both sides of the story.
Here are some questions people also ask about benzodiazepine addiction treatment, as well as benzodiazepine addiction more generally.
Studies estimate that approximately 40% of people who take benzodiazepines daily for six weeks or longer will develop physical dependence. Among long-term users, around 17% meet the criteria for benzodiazepine use disorder. The risk increases significantly with higher doses, longer duration of use, and a personal history of substance use or anxiety disorders.
Benzodiazepine addiction is treated through a medically supervised taper, which gradually reduces the dose to minimize dangerous withdrawal symptoms. This is typically followed by residential or outpatient treatment that includes behavioral therapy, dual diagnosis support, and relapse prevention. Because benzos are often used to manage anxiety or trauma, lasting recovery usually requires addressing the underlying mental health conditions as well.
Benzodiazepine addiction often looks like taking more than prescribed, feeling unable to function without the medication, and experiencing anxiety or physical symptoms when a dose is missed. Many people become socially withdrawn, experience memory and concentration problems, and find themselves preoccupied with ensuring they always have enough medication. Because benzos are frequently prescribed, dependence can develop gradually and go unrecognized for months or years.
Short-acting benzodiazepines like alprazolam (Xanax) and triazolam (Halcion) carry the highest abuse potential due to their rapid onset and intense but brief effect. The quick relief they produce makes them more likely to be taken more often or in higher doses than prescribed. Diazepam (Valium) also has significant abuse potential due to its potency, though its longer half-life produces a slower, more gradual effect.
The most commonly used medication for benzodiazepine withdrawal is diazepam (Valium) or chlordiazepoxide (Librium), which are longer-acting benzodiazepines used in a controlled taper to ease the transition off shorter-acting drugs. In some cases, phenobarbital or carbamazepine may be used, particularly for patients who cannot tolerate a benzo taper. All withdrawal management should be medically supervised, as benzo withdrawal can cause life-threatening seizures.
Physical dependence on benzodiazepines can develop in as little as two to four weeks of daily use at therapeutic doses. At higher doses, dependence can form even faster, sometimes within days. This is why benzodiazepines are generally recommended only for short-term use, and why stopping them should always be done gradually under medical supervision.
The safest and most effective way to stop taking benzos is through a slow, medically supervised taper that gradually reduces the dose over weeks or months. Stopping abruptly or too quickly can trigger severe withdrawal symptoms, including seizures, which can be life-threatening. Working with a treatment team that can manage both the physical taper and the underlying anxiety or mental health needs gives you the best chance of a successful, lasting recovery.
Benzodiazepine withdrawal symptoms include intense anxiety, insomnia, irritability, sweating, tremors, muscle pain, and heart palpitations. In more severe cases, withdrawal can cause hallucinations, delirium, and grand mal seizures. Symptoms typically begin within 24 hours for short-acting benzos, or up to a week after stopping longer-acting ones, and can persist for weeks or months in a phase known as protracted withdrawal.
Acute benzodiazepine detox typically lasts one to two weeks, though this varies depending on the specific drug, dose, and duration of use. Long-acting benzos like diazepam may produce withdrawal symptoms that peak later and last longer than short-acting ones like Xanax. Some people experience protracted withdrawal syndrome, where milder symptoms such as anxiety, insomnia, and cognitive fog persist for several months after stopping.
The body eliminates benzodiazepines through the liver and kidneys, and there is no safe shortcut to speed up this process. Staying well-hydrated, eating nutritiously, and getting adequate sleep supports the body’s natural detox processes. The safest approach is a medically supervised taper that allows the body to adjust gradually, rather than attempting to flush the drug out quickly, which can trigger dangerous withdrawal.
Going cold turkey off diazepam is strongly discouraged and can be life-threatening. Because diazepam is a long-acting benzodiazepine, abrupt cessation can trigger severe withdrawal symptoms including seizures and delirium, sometimes days after the last dose. Medical supervision and a gradual taper are essential for safely stopping diazepam, especially after prolonged or high-dose use.
Because diazepam has a long half-life and active metabolites that remain in the body for days, acute withdrawal symptoms may not peak until one to two weeks after the last dose. A full medical detox from diazepam, including a supervised taper, typically takes four to eight weeks depending on the dose and duration of use. Some individuals experience lingering symptoms such as anxiety and sleep disturbances for several months beyond the initial detox period.
Benzo flu is a colloquial term for the flu-like physical symptoms that commonly occur during benzodiazepine withdrawal, including fatigue, body aches, sweating, nausea, and headaches. These symptoms result from the nervous system recalibrating after prolonged suppression by the drug. Benzo flu typically occurs in the early stages of withdrawal and can last from a few days to several weeks depending on the individual and the taper schedule.
Benzo belly refers to the gastrointestinal distress, including bloating, cramping, nausea, and digestive irregularity, that many people experience during benzodiazepine withdrawal and early recovery. It occurs because benzodiazepines affect GABA receptors throughout the body, including in the gut, and the digestive system takes time to regulate after dependence. Benzo belly can persist for weeks to months but typically improves gradually as the nervous system stabilizes.
Starting recovery from benzodiazepines can feel overwhelming, especially when withdrawal, anxiety, and uncertainty make it hard to imagine life on the other side. But you’re not alone in this. At Ojai Recovery, we believe that healing begins with feeling safe, supported, and understood.
That’s why we’ve designed the first step to be simple, pressure-free, and rooted in compassion, so you can begin your journey with confidence and clarity. This is your space to pause, breathe, and begin again. Let’s leave the fear behind and start building a life that feels steady, clear, and truly yours.
Fill out the form below and we’ll be in touch shortly. We’ll listen, answer your questions, and help you explore the options that feel right for you.